(From Fibromyalgia
Network, January 1995)
Are problems such as
facial pain, jaw pain, headaches, ear pain, neck/shoulder pain,
and the feeling of muscle weakness ganging up on you? Patients with
fibromyalgia and chronic fatigue syndrome who have a TMJ disorder
would answer YES to this question. What follows is an explanation
of why these symptoms might be wearing you thin and a list of suggestions
on how you might "off-load" these burdens to ease your overall discomfort.
Temporomandibular joint
disorder (TMJD) expert and pathologist Herbert Gordon, D.D.S.,
Ph.D., who practices in Seattle, WA, offers this story
his grandfather told him years ago to demonstrate how pain impacts
your sense of well-being:
"A man went to a doctor,
saying, 'I need your help.' The doctor responded, 'What's wrong?'
The man said, 'My ankles are not doing well, my knees hurt, my back
hurts, my stomach hurts, my ears hurt, my chest hurts, my head hurts,
my tongue hurts ... and I myself don't feel so good either!'"
FMS/CFS patients suffer
from constant pain arising from multiple body sites, much like the
man in Dr. Gordon's story. Naturally, the more areas of pain a person
has, the more rotten they are likely to feel. Learning how to focus
in on troublesome symptoms so as to minimize their impact can be
done with the assistance of your health care team and a little understanding
about various types of regional pain syndromes, body posture mechanics,
and the way pain signals are processed in the brain.
Regional
Pain Syndromes
Myofascial pain syndrome
(MPS) is a term used for the kind of muscle pain found in multiple
body sites in FMS/CFS patients. In MPS, trigger points (rather than
tender points) occur, causing pain at distant sites. There are a
number of MP syndromes and a multitude of myofascial trigger points
throughout the body. The head, neck, upper back, and shoulders are
particularly active. A common form of MPS involves the jaw movement
muscles and is called temporomandibular joint disorder (TMJD).
When a referred pain
phenomenon is present, the source of the pain can be confusing.
A tooth ache may not be caused by a cavity: "If the pain originates
in one of the jaw movement muscles like the temporalis," says Dr.
Gordon, "extracting the sore tooth won't alleviate the problem."
Another common pain referral scenario can occur in a person who
is experiencing a heart attack. This individual may also have pain
shooting down into their left arm or hand, but a person doesn't
have to have a heart problem to know what this feels like. Patients
with FMS have been reported to have trigger points in the chest
region which lead to a referral of pain down an arm as well -- somewhat
mimicking a heart attack.
To explain what might
be happening at trigger points, Dr. Gordon referenced a 1993 report
by David Hubbard, M.D., a researcher in San Diego, CA. Dr.
Hubbard inserted needle electrodes into the trigger points of the
trapezius muscle (back shoulder area) and another one simultaneously
into a nearby non-tender spot in the same muscle in three different
study groups: patients with muscle tension headaches (a form of
MPS), patients with FMS, and healthy individuals. He had the two
electromyographs (EMGs) going at the same time and measured the
neurological activity at both muscle locations. In the muscle tissue
away from the trigger point, there was only a low level of activity.
At the trigger point, however, the EMG signals were significantly
stronger in the two patient groups as compared to the healthy controls.
Hubbard hypothesized that trigger points are caused by sustained
sympathetic nervous system activity that causes the muscle to tense
up and produce pain.
But what if the patients
just relaxed their trapezius muscle? Wouldn't this release the tension
at the trigger point? When Hubbard asked the patients to relax,
the EMG amplitude at the non-pain site decreased, demonstrating
that patients could relax their muscles upon command. Yet,
the EMG signals at the trigger points didn't decrease.
"So it appears that
when patients purposely relax, they aren't fully relaxed at the
trigger points," says Dr. Gordon. "The muscle will stay tense as
a result" ... and it will require more than relaxation therapy to
ease the pain.
Patients who have TMJD
or other regional pain syndromes should seek prompt treatment. Unlike
the deep, diffuse aching caused by FMS, the pain of MPS is often
treatable in a variety of ways (see TMJ Disorders Update below).
Underscoring the importance of treatment, Gordon says, "A large
area of your brain is set aside for controlling mouth and jaw movements,
speech and chewing. If you have pain in jaw movement muscles or
an abnormal temporomandibular joint with clicking or popping and
pain, you are going to tie up a significant amount of your brain
in a painful process. Current research in chronic pain has shown
that the longer the pain exists in a particular site, the more involved
the brain becomes, and the area of the brain that deals with pain
grows larger. This is why existing areas of diagnosable pain need
to be treated as promptly as possible in order to reduce the overall
burden on the brain and the rest of the body. This is especially
important in FMS/CFS."
Body
Mechanics
Maintaining good posture
is important. "If you carry your body incorrectly, you are going
to induce strain," says Gordon. "If you induce strain, you are hurting
the muscles, ligaments and tendons." Just holding up your head in
a proper position may not be easy to do when you are tired, your
neck and shoulders hurt, and your postural muscles have begun to
weaken due to a decreased activity level--a situation often imposed
by FMS/CFS.
What happens if you
don't hold your head upright? According to Dr. Gordon, for each
inch that you bend your head forward and keep it in a forward position,
the weight of your head doubles! The additional weight of your head
will strain your jaw joints, neck, back and shoulder muscles, and
of course, cause more pain (including headaches).
Regardless of whether
you are sitting, standing or lying down, pay close attention to
your posture and body mechanics. If you are having problems in this
area, ask your doctor for a referral to a physical therapist or
occupational therapist.
Your
Body's Pain-Control System
By the time a pain signal
from a sore toe travels up the nerves in your leg, enters your spinal
cord, and reaches your brain, the pain signal is usually minimized,
if not completely abolished. "There are specific neurons, cells
in the spinal cord and central nervous system whose job it is to
block out pain," says Gordon. "Chemical agents in the brain have
a dampening effect on pain."
Using marathon runners
as an example, Dr. Gordon says they run until they pass through
"the wall" and reach the runner's high. How does this happen? Their
bodies produce opium-like chemicals in the brain which block out
the pain signals coming from the many muscle sites that are injured
while they are performing their run. Yes, they are in good condition,
but they are pushing their bodies and their muscles are actually
hurting...it's just that the opium-like material blocks the pain.
"If you give these runners an opium-blocking agent, they crash,"
says Dr. Gordon. "They go from a high to a feeling of painful withdrawal."
Under normal conditions,
the body is able to filter out or block pain signals that are generated
from the muscles while running a marathon. But in people with chronic
pain conditions like FMS/CFS, Dr. Gordon, as well as others in the
field, suspect that patients have lost some of their ability to
filter out pain at the spinal cord level and to block it out at
the higher regions in the brain. This is one of the effects of the
limbic system deregulation that many believe is the cause of FMS/CFS.
"Ongoing discomfort
from previous surgeries, falls, motor vehicle accidents, postural
problems, untreated pain, or incompletely treated pain for distinct
conditions should be dealt with," says Gordon, "in order to help
off-load the body's total burden of pain." When these measures are
taken to minimize regional pain problems, Dr. Gordon finds that
FMS/CFS patients feel better overall, although they are by no means
cured.
TMJ
DISORDERS UPDATE
TMJ disorders involve the muscles that move the jaw or can involve
the jaw joints as well. TMJD is the most common form of MPS and for
good reason. "The TMJ has been estimated by one person to be the most
active joint in the body," says Dr. Gordon. "It moves approximately
2000 times in a 24-hour day!" According to Gordon, there are two major
causes of TMJD: Extensive clenching or grinding of teeth and whiplash
injuries. "We all clench and grind our teeth. Those in severe stress,
and those in chronic pain, grind and clench more than usual. This
overuses the jaw muscles and places pressure on TMJ tissues. This
can lead to dislocation of the moveable disc in the jaw joint and
produce clicking, pain, and limited movement. Whiplash forces that
can injure the neck may also injure jaw movement muscles and the temporomandibular
joints. A major reason for the high prevalence of TMJD in FMS/CFS
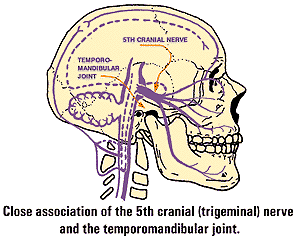
could be the association of the jaw musculature with the 5th cranial,
or trigeminal, nerve that feeds directly into the limbic system of
the brain.
Dr. Gordon explains:
"The 5th cranial nerve supplies all of the jaw movement muscles,
the temporomandibular joints, a portion of the throat, the ears,
the back of the eye and sinus cavities and the muscles on the side
of the head. Recent studies show that the 5th nerve also supplies
sensory input to the blood vessels of the brain."
"The 5th nerve," notes
Dr. Gordon, "is the communicating center for all pain arising in
the neck, head, jaw, eyes, ears, sinuses, and the cervical spine.
It may well be the center of integration of head and neck pain,
as well as jaw movement.
These facts help explain
why TMJD can have so wide an effect and be involved in headaches.
It also explains how dysfunction of jaw muscles and joints could
amplify problems in the limbic system."
Your
Treatment Options
If you have the above
symptoms of TMJD and have FMS/CFS, seek consultation with a TMJD
specialist. Your problems may be too complex for a general practitioner
of dentistry.
A diagnostic examination
is necessary to determine whether a jaw muscle problem is present
or if the jaw joints are also involved. Dr. Gordon advises that
all of the FMS/CFS patients he has seen have the more severe form
of TMJD.
Treatment includes the
use of special TMJ appliances--splints (not the usual nightguards),
exercises for the jaw muscles, diet, a variety of physical therapy
treatments, jaw mobilization (manipulation of the jaw to put out-of-place
discs into normal position), trigger point/jaw joint injections,
ultrasound, laser therapy to the TM joints, pain medications (analgesics
like ibuprofen, narcotic agents if needed), medications to aid in
sleep, as well as medications to help with muscle stiffness and
soreness. Biofeedback therapy is also utilized. All of the medications
and therapy must be coordinated with the overall treatment for FMS/CFS.
Medications commonly
used to treat TMJD include: Non-opiod analgesics (aspirin, Aleve,
ibuprofen, etc.) and muscle relaxants such as Soma (carisoprodol)
and Flexeril (cyclobenzaprine). According to Dr. Gordon, "These
are best used on a regular schedule around the clock." One pilot
study in 1991 showed that 0.25 - 1.0 mg per night of Klonopin (clonazepam)
may be helpful as well.
Dr. Gordon believes
these methods can be beneficial in 99% of cases. Surgical intervention
is needed in only 1% of cases.
Recommendations
for Self-Help:
- Rest your jaw whenever
possible. The best way is to keep your teeth apart and let your
jaw "hang" so as to relax all facial muscles. You might find that
it is not easy to relax muscles that hurt, so consult a biofeedback/relaxation
specialist for help.
- Maintain good posture.
- Stretch sore jaw muscles
2-3 times daily. At first you may not be able to fully open your
mouth. If this is due to sore muscles, heat can help. If this
is due to a joint disorder, it may cause more pain. Some patients
find that a moist hot towel or a cup of ice applied to the side
of the face can ease the pain and stiffness enough to stretch
the muscles.
- Massage of jaw, head,
neck and shoulder muscles on a regular basis can be helpful to
ease muscle tension and improve range of motion. Seek the assistance
of a licensed massage or physical therapist, or TMJD specialist.
- Chew all foods on
your molar teeth. Do not bite off food with the front of your
mouth. Dice all food to 1/4-inch sized pieces. Microwave or steam
all vegetables to soften them.
Want
to lighten your load? Become a Member of the Fibromyalgia Network
(click here).
Myofascial
Pain Dysfunction: Treatments used by ADA members, E. Glass, et al,
J Craniomandib Prac 11(1):25- 29, 1993.
Administration
of Clonazepam in the Treatment of TMD and Associated Myofascial
Pain, S. Harkins, et al, J Craniomandib Disord Facial Oral Pain
5:179-186, 1991.
(Back
to Top)
|

